pancreatic cancer
Definition
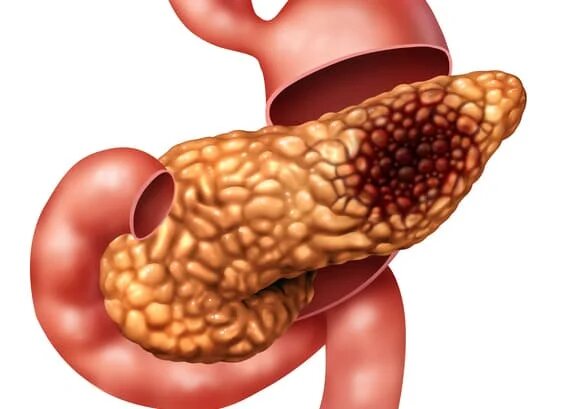 Pancreatic cancer starts in the tissues of your pancreas - an organ in your abdomen that sits behind the lower part of your stomach. Your pancreas releases enzymes that aid digestion and produces hormones that help manage your blood sugar.
Pancreatic cancer starts in the tissues of your pancreas - an organ in your abdomen that sits behind the lower part of your stomach. Your pancreas releases enzymes that aid digestion and produces hormones that help manage your blood sugar.
Many types of growths can occur in the pancreas, including cancerous and non-cancerous tumors. The most common type of cancer that forms in the pancreas begins in the cells that line the ducts that carry digestive enzymes out of the pancreas (pancreatic ductal adenocarcinoma).
Pancreas cancer is rarely detected in its earliest stages when it is most curable. This is because it often does not cause symptoms before spreading to other organs.
Treatment options for pancreatic cancer are chosen based on the extent of the cancer. Options may include surgery, chemotherapy, radiation therapy, or a combination of these.
Symptoms of pancreatic cancer
Signs and symptoms of pancreatic cancer often only appear when the disease is advanced. They may include:
Abdominal pain that radiates to the back.
Loss of appetite or unintentional weight loss.
Yellowness of your skin and the whites of your eyes (jaundice).
Dark colored urine.
Itchy skin.
New diagnosis of diabetes or existing diabetes that is becoming more difficult to control.
Blood clots.
Fatigue.
When to see a doctor
Consult your doctor if you experience any unexplained symptoms that worry you. Many other conditions can cause these symptoms, so your doctor can check for these conditions as well as pancreatic cancer.
The causes of pancreatic cancer
It is not known what causes pancreatic cancer. Doctors have identified certain factors that may increase the risk of this type of cancer, including smoking and certain inherited genetic mutations.
Understanding your pancreas
Your pancreas is about 15 centimeters long and looks like a pear lying on its side. It releases (secrets) hormones, including insulin, to help your body process the sugar in the food you eat. And it produces digestive juices to help your body digest food and absorb nutrients.
How pancreatic cancer forms
Pancreatic cancer occurs when cells in your pancreas develop changes (mutations) in their DNA. A cell's DNA contains the instructions that tell a cell what to do. These mutations tell cells to grow out of control and continue to live after normal cells die. These accumulating cells can form a tumour. When left untreated, pancreatic cancer cells can spread to nearby organs and blood vessels and to distant parts of the body.
Most pancreatic cancers start in the cells that line the ducts of the pancreas. This type of cancer is called pancreatic adenocarcinoma or exocrine cancer of the pancreas. Less commonly, cancer can form in the hormone-producing cells or neuroendocrine cells of the pancreas. These types of cancer are called pancreatic neuroendocrine tumors, islet cell tumors, or pancreatic endocrine cancer.
Risk factors
Factors that may increase your risk of pancreatic cancer include:
Smoking.
Diabetes.
Chronic inflammation of the pancreas (pancreatitis).
Family history of genetic syndromes that may increase the risk of cancer, including a BRCA2 gene mutation, the Lynch syndrome and familial atypical mole malignant melanoma syndrome (FAMMM).
Family history of pancreatic cancer.
Obesity.
Older age, as most people are diagnosed after age 65.
A large study has shown that the combination of smoking, long-standing diabetes and poor diet increases the risk of pancreatic cancer beyond the risk of any of these factors alone.
Complications
As pancreatic cancer progresses, it can lead to complications such as:
Weight Loss. A number of factors can cause weight loss in people with pancreatic cancer. Weight loss can occur when cancer consumes the body's energy. Nausea and vomiting caused by cancer treatments or a tumor pressing on your stomach can make eating difficult. Or your body may have trouble processing nutrients from food because your pancreas isn't producing enough digestive juices.
Jaundice. Pancreatic cancer that blocks the bile duct from the liver can cause jaundice. Signs include yellow skin and eyes, dark-colored urine, and light-colored stools. Jaundice usually occurs without abdominal pain.
Pain. A growing tumor can press on nerves in the abdomen, causing pain that can become severe. Painkillers can help you feel more comfortable. Treatments, such as radiation therapy and chemotherapy, can help slow tumor growth and relieve pain.
In severe cases, your doctor may recommend a procedure to inject alcohol into the nerves that control pain in your abdomen (celiac plexus block). This procedure prevents nerves from sending pain signals to your brain.
A bowel obstruction. Pancreatic cancer that grows or presses on the first part of the small intestine (duodenum) can block the flow of digested food from your stomach to your intestines.
Your doctor may recommend that a tube (stent) be placed in your small intestine to keep it open. In some situations, it may help to have surgery to place a temporary feeding tube or to attach your stomach to a lower point in your intestines that isn't blocked by cancer.
Prevention
You can lower your risk of pancreatic cancer if you:
Quit Smoking. If you smoke, try to quit. Talk to your doctor about strategies to help you quit, including support groups, medications, and nicotine replacement therapy. If you don't smoke, don't start.
Maintain a healthy weight. If you are at a healthy weight, work to maintain it. If you need to lose weight, aim for slow, steady weight loss - 1 to 2 pounds (0.5 to 1 kilogram) per week. Combine daily exercise with a diet rich in vegetables, fruits and whole grains with smaller portions to help you lose weight.
Choose a healthy diet. A diet rich in colorful fruits and vegetables and whole grains may help reduce your risk of cancer.
Consider seeing a genetic counselor if you have a family history of pancreatic cancer. He or she can review your family health history with you and determine if you might benefit from genetic testing to understand your risk for pancreatic cancer or other cancers.
What treatments are available?
In 10 to 20% of cases, it is possible to remove the tumor by surgery with the aim of curing the disease. It is a complex operation, most often completed with chemotherapy 4 to 8 weeks later.
Surgical resection of the tumorous part of the pancreas is the basis of curative treatment for pancreatic cancer. It is only possible if the tumor remains localized in the pancreas without having spread tumor cells into other organs, responsible for the formation of daughter tumors called metastases.
The most common sites of pancreatic metastases are the liver and lungs. Their research is part of the pre-operative assessment of pancreatic cancer carried out by chest and pelvic abdominal CT scan, to which a PET scan can be added if necessary (injection of a sugar marked with a radioactive tracer which will bind to the dividing tumor cells).
Local peripancreatic invasion of neighboring organs or vessels can either prove to be resectable with the tumor by more complex surgery with venous vascular reconstructions (invasion of the superior mesenteric vein, portal vein or the splenic vein) or constitute a contraindication to surgical excision which is sometimes only identified during the intervention leading the surgeon to give up pancreatectomy in favor of other surgical procedures intended to treat the symptoms: biliary diversion to treat jaundice by restoring a circuit for bile, gastric bypass to avoid digestive occlusion by the tumour.
Chemotherapy uses anti-cancer drugs that act throughout the body on all cancer cells, including those that are not detected by examinations. It may require the placement of an implantable chamber. GEMCITABINE is now routinely offered after curative resection of pancreatic cancer. It has shown its effectiveness in reducing the risk of recurrence. The duration of this treatment is 6 months. This product is also offered in the event of an unresectable tumour. Other chemotherapies can then also be used.
If the tumor is not operable, chemotherapy, combined in some cases with radiotherapy, can help slow the development of the disease, relieve symptoms (reduce pain in particular) and improve the quality of life.
The tumor can obstruct the flow of bile to the intestine causing itching and jaundice. In this case, it is necessary to drain the bile by placing a stent endoscopically or by performing a bypass by surgical operation.
The procedure involves the removal of part of the stomach, the gallbladder, part of the bile ducts, the head of the pancreas and the entire duodenum.
What is tracking?
Follow-up depends on the stage at which your cancer was diagnosed and the treatment you received. The schedule and duration are determined with your doctor in collaboration with the specialized team that carried out the treatment. Long-term monitoring after pancreatectomy for pancreatic cancer is based on regular check-ups, most often combining clinical examination with blood assays for ACE and CA 19-9 and radiological examination of the abdomen (ultrasound, scanner, MRI) and lungs. A nutritional follow-up is set up as soon as possible.
Your doctor will also tell you the signs that should lead you to urgent medical attention: itching and jaundice in particular.
The occurrence of a recurrence of the cancer, local intra-abdominal or distant metastatic is possible even beyond 10 years after the initial surgery only very rarely justifies a reoperation. Its treatment is based on chemotherapy possibly associated with radiotherapy.
The various doctors involved in monitoring keep each other informed. In some cases, you may be offered access to specialized palliative care teams.