Rupture of the cruciate ligament of the knee
What is it about ?
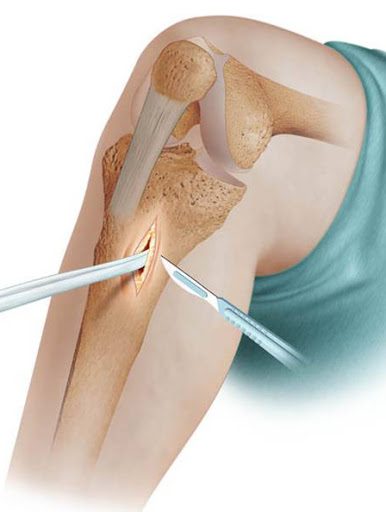 The stability of the knee is ensured by ligaments which are kinds of more or less elastic stays keeping the articular surfaces in contact. The anterior cruciate ligament, located inside the joint, connects the anterior part of the tibia to the posterior part of the femur. It prevents the tibia from moving forward and stabilizes the knee during pivot movements.
The stability of the knee is ensured by ligaments which are kinds of more or less elastic stays keeping the articular surfaces in contact. The anterior cruciate ligament, located inside the joint, connects the anterior part of the tibia to the posterior part of the femur. It prevents the tibia from moving forward and stabilizes the knee during pivot movements.
What is anterior cruciate ligament rupture?
 Ruptures are always traumatic during torsion or during hyperextension of the knee (fall on skis, shoot in the void, etc.)
Ruptures are always traumatic during torsion or during hyperextension of the knee (fall on skis, shoot in the void, etc.)
This ligament when it is broken gives laxity to the knee joint which can, depending on your physical activities, result in joint instability causing your knee to bend.
Why a ligamentoplasty operation?
The rupture of the anterior cruciate ligament heals badly and often in a non-functional way. The repercussions on the stability of the knee are therefore frequent and variable depending on the case and above all depend on the solicitation of the knee. Indeed, certain movements (contact pivots), carried out in particular during the practice of sport, cannot be done without an effective Anterior Cruciate Ligament. This ligament injury therefore leads to instability of the joint which can result in knee bends.
These instability accidents are similar to joint subluxations that can cause damage to the cartilage, menisci and other ligaments. This dynamic malfunction of the joint eventually leads to a progressive degradation of the joint and bone surfaces leading to osteoarthritis.
The goal of ligamentoplasty of the anterior cruciate is therefore to restore good stability of the joint thanks to this ligament replacement. Thus sports activities can be resumed in good conditions and above all meniscal, cartilage and ligament degradation of the knee is avoided. The accelerated development of osteoarthritis is therefore halted.
What type of intervention for the cruciate ligament?
The ligamentoplasty of the anterior cruciate ligament involves replacing the ruptured ligament with a transplant taken from your knee. Currently 2 types of transplants are commonly used to replace your ligament:
The patellar tendon: the central 1/3 of your patellar tendon is removed with a tibial and patellar bone patch at each end of it to allow bone fixation of the transplant.
The DIDT: 2 tendons are taken from the inside of the knee at the crow's feet (the internal rectus and the semi-tendinosus), these 2 tendons are each folded in 2 and this new 4-strand ligament will replace the ruptured ACL.
Ligamentoplasty surgical follow-up
They are generally simple. There are no consequences of tendon harvesting on knee mobility. Hospitalization is on average 3 days. The support of the lower limb under cover of a boned splint is resumed immediately. This splint is to be worn for a fortnight until the muscles allow a good locking of the knee.
There is no restriction of knee mobility, flexion and extension must imperatively be worked quickly and without limitation. A good rehabilitation with a rapid recovery of mobility is the guarantee of a good functional result. However, certain rules for post-operative work are important so as not to damage the new ligament, you must discuss them with your physiotherapist in order to fully understand and integrate them.
Walking with English canes is desirable during the first 3 weeks in order to relieve your knee of the weight of the body.
In practice, the exercise bike and swimming (crawl, no breaststroke) can be started on the 45th day, running on flat ground on the 90th day, contact pivot sports on the 6th month.
The resumption of professional activities varies according to the profession. A constraining activity of the knee can only be considered from the 4th month.
Risks and complications of ligamentoplasty
A hematoma may form as a result of postoperative intra-articular bleeding. Depending on its importance, arthroscopic evacuation may be necessary.
Joint stiffness can develop if postoperative rehabilitation is not well taken care of.
Algodystrophy with joint demineralization and stiffness may occur and require appropriate treatment with calcium injections for several months.
An infection of the joint remains exceptional since the surgical procedure is performed arthroscopically. This known complication requires washing of the knee and more or less long antibiotics with follow-up treatment in the infectious diseases department.
Phlebitis by formation of a venous thrombus is a non-exceptional complication with potentially serious consequences. Follow-up of the preventive treatment of this thrombosis by daily injections of LMWH (Lovenox, Innohep, etc.) is imperative.
The risks listed above do not constitute a completely exhaustive list. Your surgeon will give you all the necessary additional explanations and will be at your disposal to discuss each particular case with you.
The expected results of ligamentoplasty
Generally, a very good result of the intervention on the mobility and stability of the knee is obtained very quickly with in particular a disappearance of blockages and painful sensations of instability. However, postoperative follow-up of a good functional rehabilitation is essential to perfect the final result.
The resumption of sports activities is generally done in the best conditions, however, the replaced ligament is not better than the original ligament and a new rupture can always occur. We must therefore remain vigilant in the face of the risks represented by contact pivot sports such as team sports, combat sports and tennis.