shoulder dislocation
What is it about ?
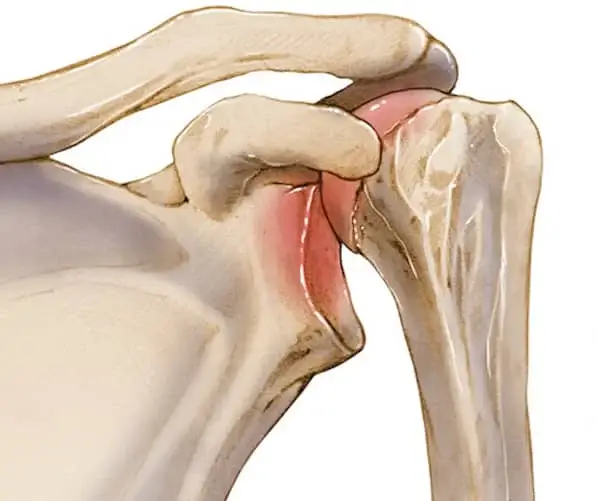 The recurrent dislocations of the shoulder is a pathology encountered in young and generally athletic subjects. Its rapid treatment is imperative to avoid joint damage, the frequency of which increases with the number of dislocations. Arthroscopic Bankart and Latarjet-Bristow surgeries meet specific criteria to treat patients in the best conditions and thus ensure a rapid return to activities.
The recurrent dislocations of the shoulder is a pathology encountered in young and generally athletic subjects. Its rapid treatment is imperative to avoid joint damage, the frequency of which increases with the number of dislocations. Arthroscopic Bankart and Latarjet-Bristow surgeries meet specific criteria to treat patients in the best conditions and thus ensure a rapid return to activities.
What is an unstable shoulder?
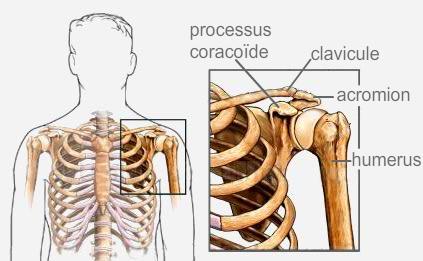 The shoulder corresponds to the glenohumeral joint between the humeral head and the glenoid of the scapula (see animation). The humeral head is permanently maintained facing the glenoid thanks to several structures: the joint capsule which is a pocket surrounding the joint, the ligaments which are a kind of shrouds connecting the glenoid to the humerus and finally the labrum which is a fibro-cartilaginous bead around the glenoid (equivalent to the menisci in the knee).
The shoulder corresponds to the glenohumeral joint between the humeral head and the glenoid of the scapula (see animation). The humeral head is permanently maintained facing the glenoid thanks to several structures: the joint capsule which is a pocket surrounding the joint, the ligaments which are a kind of shrouds connecting the glenoid to the humerus and finally the labrum which is a fibro-cartilaginous bead around the glenoid (equivalent to the menisci in the knee).
During a trauma causing a dislocation of the shoulder, these structures can be distended or ruptured (see animation opposite) resulting in instability of the humeral head during movements. The shoulder can then dislocate more or less completely during sports or even during certain gestures of everyday life. This unstable shoulder is generally the cause of chronic disabling pain in addition of course to the risk of dislocation.
The evolution of this instability is towards increasingly easy and frequent dislocations. The joint damage caused concerns the labro-capsulo-ligamentous structures but also the cartilage of the joint, the bone of the glenoid and the humeral head and finally the tendons of the rotator cuff. In certain violent dislocations, vascular and nervous lesions can even be encountered.
All of these lesions logically worsen with the frequency of dislocations
Why surgery?
The goal of surgical stabilization of the shoulder is to prevent repeated dislocations, thus preventing the progressive degradation of the joint and the functional loss of the shoulder.
This stabilizing intervention restores good joint dynamics compatible with the resumption of functional activities in good conditions.
It should therefore be considered as soon as the dislocations recur or even in the event of an unstable painful shoulder without complete dislocations.
What is shoulder stabilization?
Shoulder stabilization consists of preventing the head of the humerus from protruding from its natural location. Two surgical techniques are possible: capsular, ligament and labral suture using the BANKART technique, or placement of a bone block in front of the glenoid using the screwed coracoid bone block technique according to LATARJET.
The BANKART technique is performed arthroscopically, i.e. without opening the joint of the shoulder. Two or three small incisions of 5mm each are made around the shoulder. An arthroscope, i.e. a small camera, is introduced through one of them to visualize the entire joint and in particular the lesions of the capsule and the ligaments. Small instruments are introduced through the other incisions to perform the surgical procedure. Several anchors are impacted at the level of the glenoid. The threads mounted on these anchors are passed through the capsule and the ligaments and tied together in order to repair the lesions.
The LATARJET thrust technique requires a short incision in front of the shoulder. The coracoid process, which is located nearby on the scapula, is removed. It is then fixed in front of the glenoid by one or two screws and constitutes a bony buffer which prevents the humeral head from moving forward.
Which intervention to choose?
The choice between one or the other technique calls upon the anatomical, physiological, clinical and radiographic characteristics of the patient.
Whatever the technique used, the procedure lasts an average of 45 minutes and requires hospitalization for 2 to 3 days. The operation is generally performed under loco-regional anesthesia or under general anesthesia. The choice of anesthesia mode should be discussed with your anesthesiologist.
Risks and complications
A hematoma may form as a result of postoperative intra-articular bleeding. Depending on its importance, arthroscopic evacuation may be necessary.
Joint stiffness can develop if postoperative rehabilitation is not well taken care of.
Algodystrophy with joint demineralization and stiffness may occur and require appropriate treatment with calcium injections for several months.
An infection of the joint remains exceptional since the surgical procedure is performed arthroscopically. This known complication requires washing of the knee and more or less long antibiotics with follow-up treatment in the infectious diseases department.
Phlebitis by formation of a venous thrombus is a non-exceptional complication with potentially serious consequences. Follow-up of the preventive treatment of this thrombosis by daily injections of LMWH (Lovenox, Innohep, etc.) is imperative.
The risks listed above do not constitute a completely exhaustive list. Your surgeon will give you all the necessary additional explanations and will be at your disposal to discuss each particular case with you.
The expected results of your operation
The disappearance of pain, apprehension and feelings of instability is very fast after the operation. Recovery of mobility and muscle strength generally takes place under particularly satisfactory conditions from the 3rd month. The recurrence of instability depends mainly on the sport practiced. It is therefore necessary to remain vigilant in the face of the risks posed by sports with armed-counter-arms (volleyball, tennis, basketball, handball or rugby). The results of these techniques are very satisfactory since a stable shoulder is obtained in nearly 90% of cases for arthroscopic Bankart and in 95% of cases for the abutment. In addition, the risk of progression to osteoarthritis of the shoulder is greatly reduced on a stabilized shoulder.