Mini Gastric Bypass
What is the Mini Gastric Bypass?
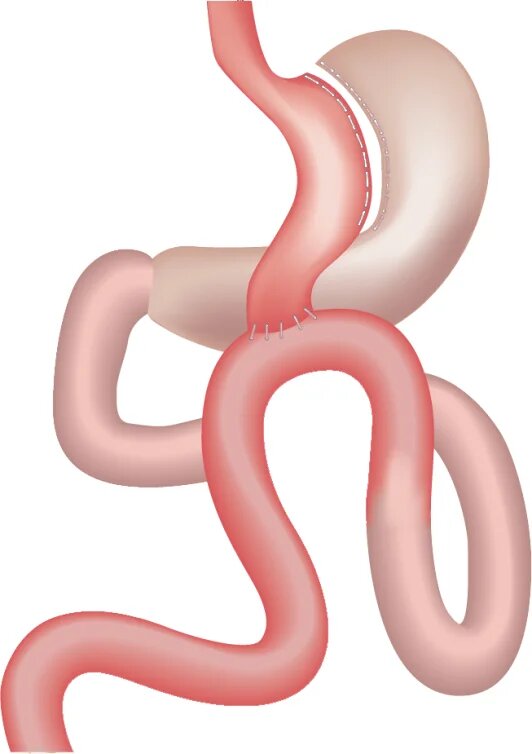 The mini-bypass, also called omega bypass, is not mini in its effectiveness but in its technique of realization. As with the classic bypass, the size of the part of the stomach through which food passes is reduced. And as with the classic bypass, the food does not pass through a part of the intestine, which is bypassed (or short-circuited). The difference is that to obtain this result the mini-bypass requires only one anastomosis (suture) of the intestine instead of two.
The mini-bypass, also called omega bypass, is not mini in its effectiveness but in its technique of realization. As with the classic bypass, the size of the part of the stomach through which food passes is reduced. And as with the classic bypass, the food does not pass through a part of the intestine, which is bypassed (or short-circuited). The difference is that to obtain this result the mini-bypass requires only one anastomosis (suture) of the intestine instead of two.
Advantages
Intervention technically easier than the classic bypass (between 45mn and 1h)
Effective in binge eating (big eaters during meals) as in nibblers
The consequences of a leak (fistula) on one of the digestive sutures are less serious than after a sleeve
Lower long-term occlusion risk than conventional bypass
Mini bypass post-operative advice
The length of hospitalization is usually 4 to 5 days before being able to return home. There is no need for a convalescent home except in special cases. Patients are allowed to take liquid food the day after the operation and mobilization is very early, at best the same evening.To the usual hyper-coagulability of the post-operative period is added in the obese an imbalance of coagulation (lower level of antithrombin III and reduced fibrinolytic activity). These are subjects at high risk of thrombosis. Pulmonary embolism is the leading cause of death in bariatric surgery. In addition to early rising, the prevention of thrombosis is done by subcutaneous injection of low molecular weight heparin at a preventive dose. Most generally, this intervention is not very painful in the postoperative period and responds well to the simple analgesics that will be given to you. prescribed when you leave the hospital. Patients are encouraged to resume light activity when they return from hospital, which is one of the advantages of laparoscopic surgery compared to laparotomy (large scar). The duration of stopping professional activities from 2 to 4 weeks is to be discussed in preoperative consultation taking into account the particular case of each patient and the nature of his work. Sports activity can, in general, be resumed after 1 month after the intervention. After an early departure from the establishment around the 4th or 5th day, the patients are seen again in surgical consultations 1 month later. The patient will then be seen every 3 months to 6 months for the first 2 years, a period to be adjusted according to the problems that may arise. Post-surgical dietary management is essential insofar as gastroplasties require an adaptation of the diet.Psychological monitoring of the patient post-operatively is not systematic, it will be done in the event of a request for support from the patient, psychiatric decompensation linked to the modification of body image and the modification of food intake. or in the event of poor behavioral adaptation to the ring (sweateater for example). mashed potatoes in flakes: it must be fairly fluid not too thick), compotes, yoghurts, cottage cheese, baby food. The 2nd and 3rd week the food should be of "tender" texture=texture of the cooked apple, ratatouille, scrambled eggs, .Choose foods that are neither too dry nor too stringy. From the 4th week, the diet returns to normal but keeping in mind that tolerance to each food is very variable. person to person:chicken may not fit at all in one person and may be fine for someone else without any problems. At the start you will have to “grope”, not only on the nature of the food but also on its volume, its size. If the food does not pass after being chewed, as a last resort, you can eat it in the form of a puree, in small pieces or mixed. Away from the operation, the hygiene and dietary rules remain important. Food intake must be regular with three meals a day and sometimes small snacks between these three main food intakes. But these snacks must remain limited and occasional and the fact of having several small meals between the main meals must be avoided. It is also important to chew properly and for a long time before swallowing. Each bite should be chewed 15-20 times before swallowing. It is also important to allow sufficient time for the meal, if necessary 30-45 min. Patients should not drink during the meal. It is necessary to try to limit oneself during the meal to the intake of food, without drink.The purpose of this way of doing things is to keep food in the gastric tube for as long as possible and therefore to obtain a better feeling of satiety. It also reduces the risk of impaction of food at the exit of the tube, which could cause pain and vomiting. Liquids should therefore be taken 10 to 15 minutes before a meal. Suitable liquids are water, tea, coffee and slightly diluted juices. Large amounts of sweets and high-calorie liquids should be absolutely avoided. Repeated intake of high calorie liquids, such as Coca-Cola, Sprite. for example, can lead to no weight loss after the procedure. Carbonated drinks (Vals, Badoit.) should be avoided because they cause stomach dilation which can lead to digestive discomfort and pain. excess skin or uneven weight loss.
The disadvantages
Recent intervention, whose short-term results are as good as those of the classic bypass and better than those of the sleeve, but with medium and long-term results unknown (intervention performed for 2-3 years not yet validated by the High Authority health)
Risk of gastroesophageal biliary reflux (1 to 3%) requiring conversion to classic bypass
Risk of ulcer of the anastomosis (suture) between the stomach and the intestine
Because of this risk of ulcer, not recommended for patients on long-term antiaggregants ( Aspirin®, Kardégic®, Plavix® or equivalent)
Risk of stenosis of the anastomosis (suture) between the stomach and intestine requiring one or more endoscopic dilations
Nutritional deficiencies (vitamins A, B6, B9, B12, D; iron; calcium; zinc) requiring oral substitution
Risk of dumping: discomfort (nausea, cramps, sweating and diarrhea) occurring after excessive absorption and /or too fast sugars, which can be corrected by dietary measures
Mini Bypass for which patients?
Patients without a tendency to gastroesophageal reflux
In case of snacking and sweet eating
What are your BMI and IMG indexes ?
Tests to do before a Mini bypass
Blood group. Full blood count. Serum Urea. serum creatinine. Protidemia and protein electrophoresis. Serum electrolytes. Calcemia. Cholesterol. Triglycerides. HDL, VLDL. Low cortisol at 7 a.m. Thyrostimulin T4. FSH. LH.
Osogastroduodenal endoscopy.
Electrocardiogram - Cardiac Ultrasound.
Abdominal ultrasound.