Polypectomy
Definition
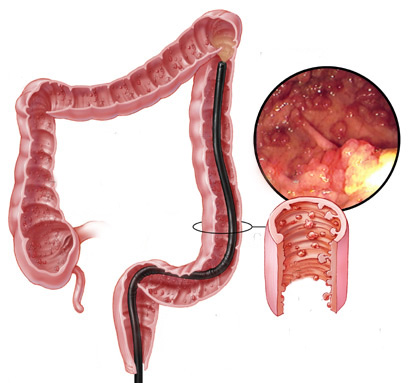 A polypectomy is a medical procedure to remove polyps that can form in any part of the digestive system, including the colon. Today, in most cases, polypectomy takes place endoscopically, often already during an exploratory colonoscopy. The alternative to this technique is open abdominal surgery.
A polypectomy is a medical procedure to remove polyps that can form in any part of the digestive system, including the colon. Today, in most cases, polypectomy takes place endoscopically, often already during an exploratory colonoscopy. The alternative to this technique is open abdominal surgery.
Why undergo a polypectomy?
Intestinal polyps are soft bumps that form on the lining of the intestines, especially in the colon and rectum. Particularly frequent after 50 years, some of these polyps, called adenomas, can go against a slow (generally 5-10 years) but inexorable malignant evolution, or in any case cause various disorders such as bleeding or intestinal obstruction .
Today, it is now established that the majority of malignant tumors of the intestine derive from polyps. The chances of a polyp developing into a malignant tumor can be quantified based on the characteristics of the polyp itself, seen during colonoscopy; if these characteristics require its removal, the doctor may decide to perform it immediately, without it being necessary to redo the endoscopic examination.
The choice of whether or not to perform polypectomy operations from the outset is influenced by the characteristics of the polyp and those of the patient, which together make it possible to quantify the risk of bleeding. If this appears concrete, the patient will be invited to undergo a polypectomy during a subsequent session.
Performing the exam
The intervention of polypectomy generally takes place in the Day Hospital regime, after carrying out a limited number of biological examinations.
During the examination, the patient is normally lying on the left side, more or less deeply sedated by the oral or intravenous administration of drugs which help to make the examination less painful and more bearable. Based on the assessment of the individual clinical case, the medical staff can decide on the degree of sedation needed or even suggest performing the procedure under general anesthesia.
As during a normal exploratory colonoscopy, the instrument (the colonoscope) is introduced through the anus and moved up, if possible, to the ileocecal valve and/or to the last ileal loops.
In order to distend the intestinal walls and facilitate visual examination, air is introduced into the colon through the colonoscope, air which can cause some discomfort even at the end of the examination. The insufflation of air, in particular, can cause swelling and painful tension in the abdomen, as well as a feeling of need to evacuate.
Once the polyp to be removed has been identified, the technique generally involves moving back at the base of the peduncle, with the help of a particular electric scalpel in the shape of a slipknot. Thanks to this instrument, capable of strangling the polyp at the base, electrical impulses are transmitted which cut and coagulate the tissues at the same time, thus helping to stop the bleeding. Once sectioned, if possible, the polyp is recovered for histological examination.is and trachea region, as well as the main bronchi in patients with a tracheostomy tube.
Not all polyps are stalked; those sessile, for example, are completely stuck to the wall of the intestine and in this case it may be necessary to detach them piece by piece, thus repeating the colonoscopy several times. When the polyp is very large or has no stem, the doctor may decide to inject a vasoconstrictor drug, such as adrenaline, into the base of the polyp, which reduces the risk of bleeding. An injection of Indian ink diluted in a saline solution (tattooing) can also be performed on the sampling site, in order to facilitate endoscopic checks and/or subsequent surgical interventions.
Whatever the polypectomy technique adopted, after removal the whole polyp or its fragments are - if possible - recovered and sent to the laboratory for histological analysis; by examining the characteristics of the polyp, the anatomo-pathologist can thus establish whether or not additional checks and/or interventions will be necessary. In a fortunately limited number of cases, for example, it may happen that the examination reveals the presence of tumor cells at the base of the polyp or the pedicle; in this case, the polypectomy cannot be considered decisive and surgery may be necessary to remove the section of the colon where the polyp was located. Alternatively, the so-called mucosectomy - submucosal dissection - can already be performed during the first poipectomy procedure, a technique which, together with polyps, allows the inner mucous layer of the intestinal wall to be removed. In this case, if the malignant lesions are confined to the mucous layer of the intestinal wall, mucosectomy can be considered curative.
Risks and Complications
Like all invasive procedures, polypectomy also comes with risks and complications. The most important, as expected, concern possible hemorrhagic evolutions, which occur in up to three out of 100 cases and which fortunately in most cases are self-limiting or stopped by endoscopic means. Only in rare circumstances can the blood loss be of such magnitude that it requires a blood transfusion or surgery. This is more likely with sessile (no stem) or large (>2 cm) polyps.
Another relatively common complication of polypectomy is perforation of the intestinal wall, which occurs in 0.3 to 0.4% of cases; this complication can be controlled with the suspension of nutrition associated with antibiotics, while in the most serious cases it may require immediate surgery. The risk of peritonitis is also formidable, largely limited by antibiotic prophylaxis.
The administration of sedatives can induce dizziness, nausea and fatigue, which usually resolve spontaneously within a few hours.
After the treatment, which lasts from 15 to 90 minutes, many patients complain of abdominal swelling problems, which can persist for a few hours during which they tend to decrease spontaneously; if this does not happen, the evacuation of gases can be promoted by inserting a rectal probe (a small tube in the anus).
Mucosectomy is fraught with the same possible complications as polypectomy, but with a higher incidence.
Preparation for polypectomy
Preparation for polypectomy is similar to that already seen for colonoscopy, to which we refer for more information. Briefly, from the 3/4 days preceding the examination, the person is invited to follow a diet without dairy products or waste (vegetables and fruits of any kind should not be consumed).
Before the examination, it is necessary to practice a minimum fast of 6 hours, to avoid problems of nausea and vomiting; if the exam takes place in the afternoon, a light breakfast is allowed early in the morning.
From the morning of the day before the examination, according to the doctor's prescription, it is necessary to perform colon cleansing through the use of laxatives combined with large amounts of water (ISOCOLAN and PURSENNID) .
Before the examination, it is advisable to inform the doctor of any allergies to certain medications or to latex.
According to medical indications, in the seven days preceding the polypectomy, treatment with oral anticoagulants, such as warfarin, should be suspended or in any case readjusted to avoid bleeding complications.
What to do after a polypectomy?
At the end of the polypectomy, the patient is kept under observation for a variable time depending on the degree of sedation, the clinical conditions, the size and characteristics of the polyp removed, as well as depending on the intervention undertaken. For example, endoscopic polypectomy and mucosectomy of polyps larger than one centimeter usually require 24 to 48 hours of observation in the hospital.
The patient will then be discharged as soon as the doctors deem it more appropriate. After discharge, the patient is instructed to rest completely at home for at least 24 hours, avoiding excessive exercise for four days.
Within 24 hours after the polypectomy, the patient receives a liquid diet, that is, without solid foods. Even after quitting, a light diet low in waste and solid or spicy foods is recommended for at least 48 hours, while alcohol should be avoided for at least three days.
Antibiotic prophylaxis can also be continued at home, according to medical indications.
After polypectomy, a period of false constipation is normal, because the surgery is performed on an intestine emptied of feces, which will require a few days of returning to a normal diet to fill up. After polypectomy, the immediate use of laxatives and enemas is therefore absolutely unnecessary and dangerous.
If symptoms of vomiting, fever, difficulty expelling air, or bleeding occur, it is important to prolong the fast and promptly contact the emergency room or medical facility that performed the polypectomy operation .