Biliopancreatic diversion with duodenal switch
Definition of the biliopancreatic switch
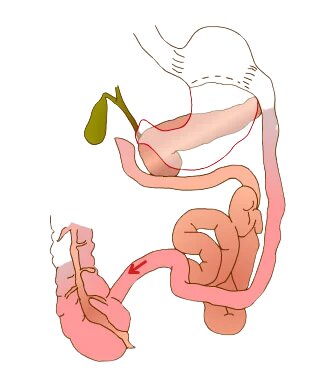 A Biliopancreatic Bypass with Duodenal Switch is a less common weight loss procedure that involves two major steps.
A Biliopancreatic Bypass with Duodenal Switch is a less common weight loss procedure that involves two major steps.
The first stage is the sleeve gastrectomy in which approximately 80% of the stomach is removed, leaving a smaller, tube-shaped, banana-like stomach. However, the valve that releases food into the small intestine (the pyloric valve) remains, along with a limited part of the small intestine that normally connects to the stomach (duodenum).
The second stage bypasses the majority of the intestine by connecting the terminal part of the intestine to the duodenum near the stomach. A BPD/DS both limits how much you can eat and reduces the absorption of nutrients, including protein and fat.
Why is it done?
This technique is made to help you lose excess weight and reduce your risk of life-threatening weight-related health problems, including:
Heart disease.
High blood pressure.
High cholesterol.
Severe sleep apnea.
Type 2 diabetes.
Stroke.
Infertility.
You must also be prepared to make permanent changes to live a healthier life before and after surgery. This can include long-term follow-up plans that involve monitoring your diet, lifestyle, and behavior, as well as your medical conditions.
The technique
The specifics of your surgery depend on your individual situation and your doctor's practices. Some surgeries are performed with large traditional or open incisions in the abdomen, while others can be performed laparoscopically, which involves inserting instruments through several small incisions in the abdomen.
The first step of a BPD/DS. The first step in a BPD/DS is to remove part of the stomach. After making the incisions with the open or laparoscopic technique, your surgeon removes a large portion of the stomach and forms the remaining portion into a narrow sleeve. Your surgeon leaves the valve that releases food into the small intestine (the pyloric valve) intact, as well as a limited part of the small intestine that normally connects to the stomach (duodenum).
The second stage of a BPD/DS. During the second stage, your surgeon makes an incision through the part of the small intestine just below the duodenum, and a second cut lower down, near the lower end of the small intestine. Then your surgeon brings the cut end near the bottom of the small intestine to the other cut end, just below the duodenum. The effect is to bypass a large segment of the small intestine.
Each part of the surgery usually takes a few hours. After surgery, you wake up in a recovery room, where medical staff monitor you for any complications.
After the surgery
Immediately after a BPD/DS procedure, you may have liquids but no solid food as your stomach and intestines begin to heal. You will then follow a special diet that slowly transitions from liquids to pureed foods. After that, you can eat soft foods and then move on to firmer foods as your body is able to tolerate them.
Your diet after surgery may continue to be quite restricted, with specified limits on how much and what you can eat and drink. Your doctor will recommend that you take vitamin and mineral supplements after surgery, including a multivitamin, calcium, and vitamin B12. These are vital in preventing micronutrient deficiencies.
You will also have frequent medical check-ups to monitor your health during the first few months following weight loss surgery. You may need lab tests, blood tests and various examinations.
You may experience changes as your body responds to the rapid weight loss in the first three to six months following BPD/DS, including:
Aches.
Feeling tired, like you have the flu.
Being cold.
Dry skin.
Thinning hair and hair loss.
Mood swings.
Results
After a BPD/DS, it may be possible to lose 70 to 80 percent of your excess weight in two years. However, the amount of weight you lose also depends on your lifestyle change.
In addition to weight loss, a BPD/DS can improve or resolve conditions often linked to being overweight, including:
Gastroesophageal reflux disease.
Heart disease.
High blood pressure.
High cholesterol.
Obstructive sleep apnea.
Type 2 diabetes.
Stroke.
Infertility.
A BPD/DS may also improve your ability to perform routine daily activities, which could help improve your quality of life.
What are your BMI and IMG indexes ?
Tests to do before a biliopancreatic switch
Blood group. Full blood count. Serum Urea. serum creatinine. Protidemia and protein electrophoresis. Serum electrolytes. Calcemia. Cholesterol. Triglycerides. HDL, VLDL. Low cortisol at 7 a.m. Thyrostimulin T4. FSH. LH.
Osogastroduodenal endoscopy.
Electrocardiogram - Cardiac Ultrasound.
Abdominal ultrasound.