Arteriovenous fistula
Definition
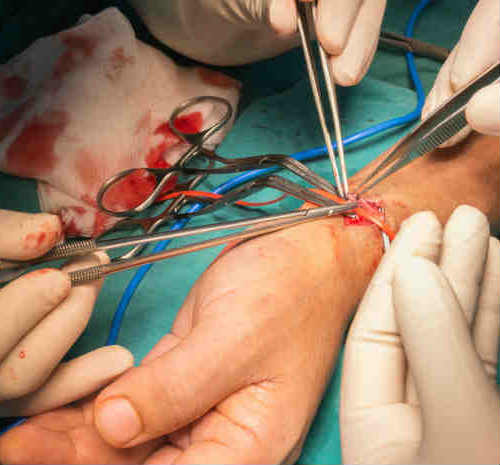 An arteriovenous fistula is an abnormal communication between an artery and a vein.
An arteriovenous fistula is an abnormal communication between an artery and a vein.
An arteriovenous fistula can be congenital (in which smaller vessels are involved) or acquired as a result of trauma (for example, gunshot or stab wounds) or a ruptured arterial aneurysm in a nearby vein. In patients with end stage renal disease requiring hemodialysis, an arteriovenous fistula is surgically created to provide vascular access for the procedure.
Symptoms
The fistula can cause symptoms and signs of:
Arterial insufficiency (eg, ulceration due to decreased arterial flow or ischemia)
Chronic venous insufficiency, caused by high-pressure arterial flow in the involved vein (eg, peripheral oedema, varicosities, stasis pigmentation)
Embolisms can pass from the venous to the arterial circulation (and cause ulceration by lodging in the distal vessels), although pressure differences make this unlikely. If the fistula is superficial, a palpable mass may be felt and the affected area is usually swollen and warm with a distended and pulsating superficial venous network.
A tremor can be palpated in correspondence with the fistula, while auscultation shows a continuous murmur (back and forth) which increases during systole.
Rarely, high-output heart failure can develop if a significant portion of cardiac output is diverted to the right heart through the fistula.
Diagnosis of arteriovenous fistula
Clinical Assessment
Sometimes ultrasoundFistulas are diagnosed clinically based on the presence of chills, murmur, and other signs. Doppler ultrasound is the best confirmatory test.
Treatment of arteriovenous fistula
Sometimes percutaneous occlusion techniques.
Sometimes surgery.
Congenital fistulas do not require treatment unless significant complications develop. If necessary, percutaneous vascular techniques can be used to place coils or "plugs" in the vessels to block the fistula. This treatment is rarely completely successful, but it often controls complications.
Acquired fistulas usually have a single major communication and can be successfully treated surgically.